Hey All!
First of all THANK YOU for all of your amazing and thoughtful questions.
I am so very honored to be a trusted source of information and encouragement for you women that are working through pelvic floor dysfunction and prolapse.
I won't be able to answer all of the questions that I received in this single blog post, but I have decided to start a series on this topic and will be answering 1-2 questions PER post.
Today's post is focused on pelvic organ prolapse or POP.
If you don't see your question answered here, DON'T WORRY! my Facebook Live later on this week and upcoming blog posts will address it. Again, you had SO MANY GREAT QUESTIONS!!!
I'd like to start off by saying that my answers to your questions come from my experience with pelvic floor dysfunction and prolapse, my training as a postnatal fitness specialist my experience training clients that have these conditions and my extensive amount of research conducted on these topics.
I am NOT a doctor of physical therapist, therefore the advice and recommendations here should ALWAYS be shared with your team of medical professionals.
I speak from my experience and my education alone.
I 100% DO NOT believe in rules and formulas when it comes to working with the pelvic floor.
There are some very helpful guidelines and effective strategies for dealing with pelvic floor dysfunction and related injuries, but I will tell you that EVERY CLIENT I SEE IN-PERSON OR ONLINE presents with pelvic floor issues slightly differently and therefore we tailor their programming to their unique problems.
You see while we know that prolapse typically presents after birth or pregnancy and we know that birth and pregnancy and risk factors for prolapse, there's a number of different factors and variables that led to the occurrence of the prolapse.
Therefore reducing symptoms and building strength (or relaxation) around the pelvic floor conditions or injuries involves using different strategies that work for different bodies, different risk factors/cause of injuries and lifestyles.
Ok! So let's get to the questions!
Question 1: " What is pelvic organ prolapse?
-Lisa
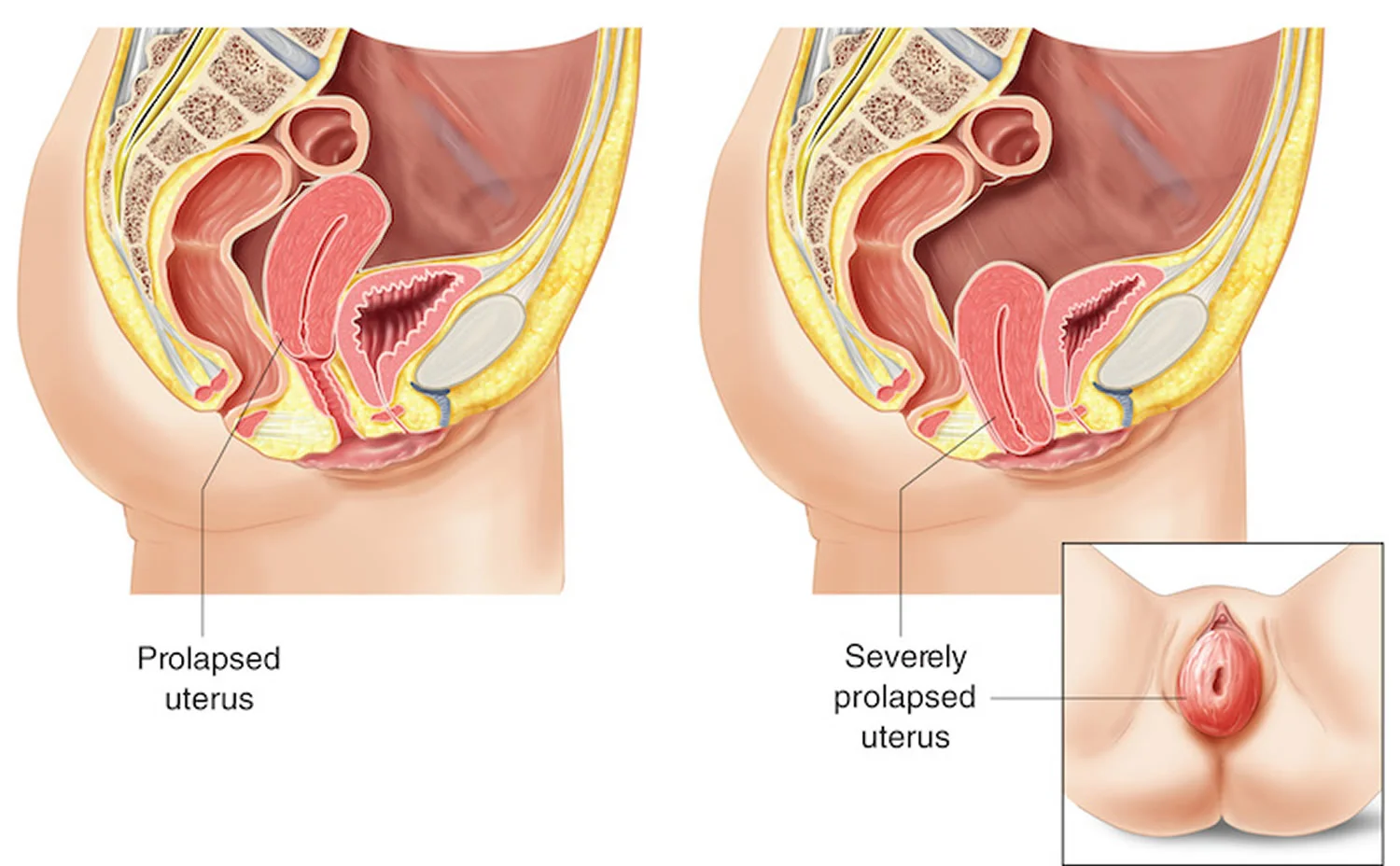
Prolapse can occur of the urethra, bladder, uterus and rectum.
Hey Lisa!! So pelvic organ prolapse (or POP) is when one or more of your pelvic organs (for women that's urethra, bladder, uterus and rectum) drops from its normal place and pushes against the walls of the vagina.
"Up to half of all parous (had a baby) women have some degree of clinical prolapse and 10-20% are symptomatic." Gyhagen et. al., 2013
So if you have prolapse and you feel alone, damaged or angry at your body, I totally get that, but try to remember that prolapse is EXTREMELY COMMON and 50% of women that have had babies have some degree of prolapse.
And while pregnancy and birth are commonly the causes of prolapse, it IS POSSIBLE for men and women that have never been pregnant or given birth to develop prolapse.
Why?
Well prolapse occurs because of strain during pregnancy, birth or postpartum life. The weakening of the muscles and or tissues that hold our pelvic organs in place. This weakening often occurs during or after pregnancy when women's ligaments and tissues are particularly stretchy.
But any activity or health condition that causes collagen degradation or consistent downward pressure on the organs can cause this as well.
That's why we see some weightlifters, singers, and gymnasts and experiencing prolapse as well as folks with a history of malnutrition, bulimia, chronic coughs, irritable bowel syndrome or inflammatory bowel disease developing prolapse.
It's all about that CHRONIC downward pressure pushing on the ligaments and tissues that eventually lose tension and give way.
How do you know if you have POP?
Often POP is described as a feeling of heaviness. A bulging sensation in or outside of the vaginal canal, but many women have prolapse and experience no obvious symptoms.
Prolapse of the bladder (most common) can effect the flow of urine, the ability to empty the bladder and the urge to urinate.
Prolapse of the rectum can cause constipation, the inability to excrete all excrement during a bowel movement, bloating and gas build-up.
Like the other two types of prolapse, prolapse of the uterus can cause pelvic pain and discomfort, feelings of heaviness and bulging, irregular bowel and urinary habits.
You can use a mirror or manually check to feel if any of your organs seem to be hanging lower than usual, which can be both education and horrifying.... but the absolute BEST COURSE OF ACTION is to have an internal exam conducted by a pelvic floor PT.
Preferably one that checks you laying down AND standing up!
I'm just scraping the surface here, go and read more on POP click here.
Question 2: "I am wondering what exercises people should not do at all when they have pelvic floor problems ? "
-Jennifer
These folks are keen to exercise right now on this beach.
Jennifer, this is a great and VERY commonly ask question.
But for real, "It depends."
If someone is experiencing "pelvic floor dysfunction" their pelvic floor can be too tight, too lax or not coordinating well.
All of these different issues call for different strategies in exercise and movement training!
This is why I ALWAYS encourage clients to see a pelvic floor physical therapist, get an internal exam and a specific diagnosis of what is going on!
For example, prolapse, a tight pelvic floor and a loose one, ALL these things can cause similar symptoms, but the prescriptive programs that help to fix the problem would all be very different!
The exercises that you want to avoid are A. the ones that make you more symptomatic and B. the ones that when you do them, you don't feel in full control of your pelvic floor, breath and alignment.
But that's really it. You will frequently here recommendations like, "Don't jump anymore." or "Never lift more than 5 lb weights." "Don't every do a deep squat" and "You can no longer run." "Do yoga."
The truth is that at the end of the day what exercises work for YOU and YOUR pelvic floor really depends on:
- your body
- your specific pelvic floor dysfunction
- the strategy you use to do the exercise
- what movements feel good (don't make you more symptomatic) and which one's do not
I personally wouldn't recommend doing a lot of jumping or heavy lifting unless you were SURE that your pelvic floor is strong and able to coordinate well with your breath and movement so that it supports your pelvic organs.
Until you feel super confident, I would also avoid exercise classes that make it impossible for you to self-regulate, pay attention to your breath and pelvic floor action and take breaks when necessary.
The best thing you can do is to get with a PT and or a coach/trainer (or both!) that is knowledgeable about the pelvic floor and can help you find the movements, lifestyle adjustments and ongoing training that makes you feel GOOD!
Question 3: "I’d be very interested in the management of pelvic organ prolapse post partum."
-Kelly
Managers.com is a thing...
Hey Kelly! I think that this is something that looks a little different for everyone.
For example what works for me and my life might not work exactly for someone else OR I may be willing to put effort into one area of healing and recovery, while someone else finds a totally different approach more impactful for their POP.
But I think that MOSTLY we can agree on the following areas should be addressed for anyone that is trying to navigate prolapse:
- See a pelvic floor physical therapist. Get diagnosed. Try out their recommended exercises. Establish a relationship with a PT that you trust, because even after your graduate from PT or if you opt to go less frequently than is recommended, you want someone to check in with intermittently to make sure that you are managing your POP well.
- Focus on your breathing and alignment.
All of us chest breathers are in the habit of taking short and shallow breaths and lose the coordination between the diaphragm and the pelvic floor.
We also tend to be tummy suckers-(suck in our bellies) with overly developed obliques or rectus abdominus muscles that struggle to relax.
Holding our bellies in and taking shallow breaths results in poor management of intra-abdominal pressure and so we are often pushing down on our pelvic organs. This is problematic for healthy pelvic floors and can either lead to POP or make existing POP worse.
If all this sounds totally new and foreign to you, then PLEASE check out Julie Wiebe's Piston Breathing Course.
Many of us with pelvic organ prolapse have a history of tilting our pelvis in a way that can either put extra strain on the pelvic floor OR cause it to become too lax to support our organs. While some degree of pelvic tilt, isn't necessarily a big deal (providing the ribs are aligned over the hips) pelvic tilts are frequently are associated with inactive glutes, another problem for pelvic floor dysfunction AND eventually POP. So CHECK how you're standing or sitting most of the day. Use this video.
- Gut health and nutrition matter. This is a frequently over-looked contributor to pelvic floor problems whether general dysfunction or POP. If your body is under-nourished, then collagen synthesis suffers. This will negatively impact all of the muscles, tissue and fascia or your body, including your pelvic floor.
Dysbiosis (imbalance of good and bad microbes) of the gut causes bloating, excessive gas, diarrhea and constipation ALL of which are STRONGLY associated with PFD and POP.
So if you're someone that is frequently struggling with any of these issues OR suspect that you might not be meeting your body's daily caloric and nutritional needs, you're going to want to prioritize restoring balance to your gut AND your diet. Learn more about how the gut and pelvic floor impact one another by checking out this OTHER POST the I wrote! Five Ways the Pelvic Floor and Gut Impact One Another.
- Get creative so that you can stay active in the ways that feel good for your mind and your pelvic floor.
I work with lots of women that come to me super frustrated that their "go to" forms of exercise for physical and mental/emotional health do not currently work for them and their pelvic floors. And I get that. There was a period of time when it seemed like every form of exercise I tried made everything worse and I was asking myself, "Am I going to be the only 36 year old doing water aerobics at the Y?"
But be patient. You don't know what's going to happen next. You don't know that you won't discover a new form of exercise that makes your pelvic floor feel just fine.
Your pelvic floor problems could dramatically improve with work and patience.
You might just find the perfect strategy that gets you back to running, yoga, pilates, lifting, or cycling.
Do what works for now and keep trying things. Don't ever give up and don't close yourself off to possibility or creativity.
Most of my fitness practice has been shaped by injury and limitations and I still have days when I have to say, "Not today, Sarah." Because my body isn't responding well.
Which brings me to my final point...
- Understand that managing POP is a process. Once you have POP, you always have it. Your symptoms and grade of prolapse may subside and reduce, but you are still at risk for it returning or worsening.
Therefore we (me included!) have to let go of the idea that this is a problem that we can FIX and totally forget about it.
I currently have no real symptoms of prolapse and both the PT and Uro-gyn say that it looks resolved, BUT there is still some weakness in the muscles of the vaginal wall and I am at a greater risk for my POP becoming symptomatic again than someone that never had it.
So I would love you to NOT have to deal with the daily anxiety and nervousness of "What if I make it worse?" .
That fear is stressful and annoying but I'm not going to tell you that you can be totally free of it, because the reality is that you're not.
I know that POP has probably stopped you from doing some of the activities that you did pre-POP and I know that you've had to change your exercise and movement strategies. You may even be at a place right now where you can't do much without feeling like you are making things worse.
Find other women that know what your struggles are.
Women that can related to your frustrations and support and encourage you, but most importantly NOT let you exclusively dwell on the negative things.
Yes your life and your body is different now and it's more than you bargained for.
It's incredibly frustrating and feels unfair. But what can you do about it?- Keep working. Keep doing those PT exercises. Set new goals.
- Believe in your body and yourself.
- Rest and put your feet up, when you can, I know I have 3 kids, it doesn't happen often....but every little bit helps. Elevated glute bridge is my preferred resting position.
- Nourish your mind and body with positive messaging, hope and nutrition. The mental struggle of POP is real and a LARGE part of the battle. I can tell you from experience that anxiety and stress is a sure way to increase your symptoms.
- Keep trying new forms of movement.
- Use a pessary sometimes to support you, so that you can move and train without worrying about making things worse.
- Surround yourself with positive messaging.
- Take care of your gut health and elimination habits. (Learn more here!)
Sarah Smith is a trainer, lifestyle coach and postnatal fitness specialist that specializes in helping women feel strong, confident and capable in their bodies!
Her specialties include kettlebells, gut health and optimization for fitness goals, pelvic floor health and function and making fitness fun! Check her out on social media here or get on her email list!! for more free content!